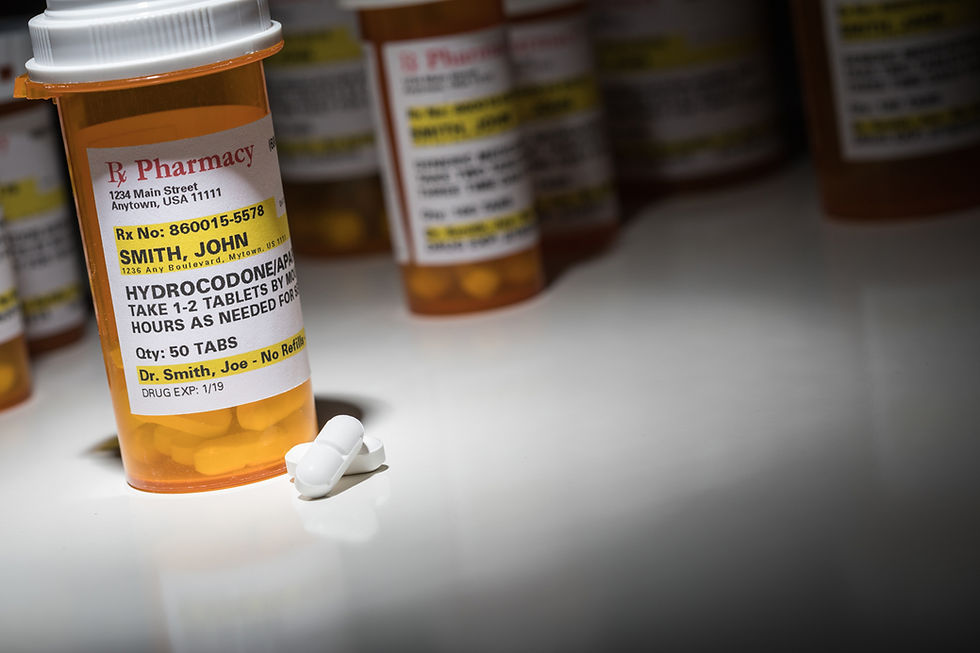
Why Regenerative Medicine is Better for Chronic Pain than Opioids
- Jul 2, 2019
- 9 min read
46 people die every day from overdoses involving prescription opioids, states a report by the CDC. Many people are prescribed opioid medications for a variety of reasons, including surgery, injury, and pain management for cancer or chronic pain. While they do work as a temporary measure for managing pain, there are many health risks associated with using opioids and they are highly addictive. Long term use of prescription opioids for chronic pain also carries the risk of death by overdose (1), because you need increasing amounts to feel the same level of pain relief. Luckily, regenerative medicine offers therapies that can heal the cause of your pain, rather than merely trying to manage it.
What are opioid medications and how do they work?
Opioids are a class of medications prescribed to treat pain, which includes Morphine, Codeine, Oxycodone, Hydrocodone, and Fentanyl. Some are naturally occurring, and others are synthetic, but they all work by interacting with opioid receptors in the nerve cells in your body.
You have these receptors because your body produces compounds such as endorphins, which work to reduce pain, anxiety, and the negative effects of stress. When opioid medications bind to the receptors, they mimic the pain-relieving action of your natural endorphins by blocking the pain signal traveling from your body to your brain. This softens your perception of pain and may also help you feel calm and relaxed.
Opioids are prescribed for pain from surgery and dental procedures, usually only for 3 to 7 days after the surgery. They are also prescribed for severe pain from cancer. Many doctors will prescribe opioid medications for managing chronic pain as well, but this is concerning because of the risks involved with long term use. Furthermore, research does not support the idea that opioids are the most effective tool for long-term pain management.
Erin Krebs, et al. conducted a year-long study in 2016, comparing opioid pain relievers with non-opioid pain relievers to discover their effects on pain-related function, pain intensity, and any adverse effects. They studied 240 patients with chronic back pain or hip or knee osteoarthritis pain and found that pain-related function was nearly the same for both groups, but pain intensity was actually lower for those taking non-opioid pain relievers. Additionally, side effects from the medication were almost double in the group taking opioid pain relievers. Krebs concluded that “Results do not support initiation of opioid therapy for moderate to severe chronic back pain or hip or knee osteoarthritis pain” (2).
Side effects of long-term opioid therapy.
Constipation, sleepiness, confusion, nausea, and vomiting are common side effects of opioids. Life-threatening side effects include shallow breathing, slowed heart rate, and loss of consciousness. Addiction and overdose are a major concern with continued use.
Opioids also modify the way your brain processes pain. With long-term use, your body becomes dependent on the medication and loses some of its natural ability to fight pain. When you do quit taking the opioids, it is common to have increased feelings of pain until your body recovers from its dependence.
In 2012, a group of doctors reviewed studies on potential adverse effects of long-term opioid therapy. This review found that long-term use negatively impacts many of the body’s systems and has led to an increasing number of deaths due to opioid overdose. They concluded that “chronic opioid treatment for noncancer pain is associated with diverse adverse effects across many organ systems.” Opioid therapy for chronic pain was discovered to harm the body in the following ways (1).
The Gastrointestinal (GI) System
25% of patients experienced nausea and 40 to 45% experienced constipation which then requires anti-nausea medications and stool softeners or laxatives. Opioid therapy can also cause vomiting, abdominal cramps, bloating, bowel obstruction, and even GI bleeding. Constipation reduces a person’s quality of life and one-third of patients with chronic constipation reported depression and psychological distress.
The Respiratory System
As many as 75% of patients using opioids around the clock for over 6 months experienced sleep disordered breathing which includes central sleep apnea, ataxic breathing, hypoxemia, and carbon-dioxide retention. Those with severe sleep apnea usually endure a far lower quality of life. Respiratory depression, bradycardia, and hypotension are life-threatening side effects which may occur with overdose. Since people need ever increasing doses to feel the same amount of pain relief, an overdose can happen without realizing you are at risk.
The Cardiovascular System
When opioid therapy was compared to NSAIDs and COX-2 inhibitors, “opioid therapy was associated with a 77% increased risk of cardiovascular events (eg, myocardial infarction, heart failure)” (1). Risk of myocardial infarction and cardiovascular revascularization were also higher than that of the general population.
The Central Nervous System
Comorbid clinical depression was 38% higher in patients on chronic opioid therapy. Dizziness and sedation are common effects, which lead to increased risk of falls and fractures. Interestingly, heightened sensitivity to pain was also common.
The Musculoskeletal System
An increased risk of fractures is a significant adverse effect, with higher doses leading to higher risk, especially among the elderly. This is concerning because “overall mortality has remained at a notably high level of 21.9% after 1 year [of a hip fracture]. Furthermore, those who do survive such an event often do not regain their health-related quality of life” (1).
The Endocrine System
Both male and female endocrine systems are strongly impacted by chronic opioid therapy. Males may experience fatigue, sexual dysfunction, infertility, hypogonadism, and decreased testosterone levels. Decreased testosterone may increase the risk of insulin resistance and metabolic syndrome. Testosterone rebuilds healthy tissue, so decreasing testosterone levels also inhibits your body’s ability to repair itself, feeding the cycle of damage that causes pain.
Females may have decreased circulating levels of estrogen and follicle-stimulating hormone, with increased prolactin. This can lead to osteoporosis, oligomenorrhea (infrequent menstruation), and galactorrhea.
The Immune System
Many types of opioid medications have immunosuppressive effects. One consequence of this effect is a higher incidence of pneumonia in elderly patients on opioid therapy (3).
Conventional medicine’s alternatives to opioid therapy.
With such a wide array of harmful possible side effects, why are opioid pain relievers prescribed so often for chronic pain? Are there no better options?
There are other therapies available, and most medical literature does recommend that you use opioid therapy only after nothing else works.
Nondrug therapies for chronic pain include biofeedback, physical therapy, spinal manipulation, massage, and acupuncture. Nerve blocks, injections, and implants are also options for pain management. Other medications such as NSAIDS or cannabinoids may be prescribed.
Unfortunately, many people spend years trying to fix their pain in a variety of ways, only to end up relying on opioids to manage it. As time goes on, their dose usually increases to achieve the same results, and additional medications are often required to combat the various side effects caused by the opioids.
Regenerative Therapies Can Heal the Cause of Your Chronic Pain.
There are many causes of chronic pain, from rheumatoid arthritis, osteoarthritis, and fibromyalgia to injuries, nerve damage, and headaches. Obviously, treatment for each of these will vary, but regenerative and functional medicine offers hope for healing, reversing damage, or minimizing the symptoms of many conditions that cause chronic pain.
Regenerative Medicine focuses on stimulating your body to repair itself, in contrast to relying on pain medication to mask the pain or resorting to surgery. At Temecula Center for Integrative Medicine, we use four scientifically proven therapies to stimulate your body’s natural healing abilities: Ozone, Ozone Clot Matrix, Stem Cells, and Pulsed Electromagnetic Field (PEMF). Depending on your unique situation, we will create a treatment plan which may also utilize supplements, dietary and lifestyle changes, massage therapy, chiropractic care, acupuncture, and naturopathic medicine to heal the cause of your chronic pain.
After a thorough evaluation, every aspect of your treatment is carefully planned to maximize the healing benefit of each therapy. Diet may be an important focus because it plays a huge role in inflammatory diseases and many other conditions. Acupuncture and massage therapy reduce pain and inflammation and have an additional benefit of releasing endorphins, which act as natural pain relievers. Chiropractic care properly aligns the body's musculoskeletal structure, restoring mobility to joints and enabling the body to heal itself without surgery or medication. The act of manipulating joints also stimulates the body to repair nearby tissue.
Ozone therapy stimulates your body to heal in many ways. It offers oxygen to cells which boosts healing of tissue, decreases inflammation and the presence of scar tissue, stimulates degenerated and damaged joints to regenerate, and enhances the immune system.
Ozone Clot Matrix (OCM) combines ozone therapy with a type of PRP (platelet-rich plasma) therapy. PRP uses the platelets in your own blood to speed up recovery times. Specific proteins in platelets, called growth factors, activate your body’s biological healing process to mend and regenerate tissue. One of the benefits of PRP is reduced scar tissue, which allows greater function and reduces chronic pain from the injury.
Ozone Clot Matrix uses your whole blood, clotting it to activate the platelets and release the growth factors. The clot is mixed with Ozone and a B-vitamin mixture, which provides oxygen-rich red blood cells and nutrients for the stimulated white blood cells to help in cleaning up damaged tissue. The advantage of using OCM rather than PRP is a longer period of regeneration, as it actively stimulates healing for two weeks, rather than 24 hours, and promotes the healing process for up to six weeks.
Stem Cell Therapy boosts your own stem cells to work more effectively to induce healing, regenerate tissue, reduce inflammation and pain, and improve function. There are thousands of clinical trials underway to discover which diseases and conditions will respond to stem cell therapy. It may be helpful in healing a wide range of conditions, from joint injuries and heart conditions to multiple sclerosis, rheumatoid arthritis, and autism.
The combination of OCM and stem cell therapy has been found to be highly effective in reducing pain and improving function in joints affected by osteoarthritis. Ozone, OCM and/or stem cell therapies have been used beneficially in our office for injuries to joints, torn muscles, non-healing fractures, fasciitis (particularly plantar fasciitis), TMJ, and bursitis.
In PEMF (Pulsed Electromagnetic Field) therapy, we place a device which uses a resonating magnetic field (RMS) over the site of pain or injury. It emits low-level electromagnetic pulses at specific frequencies which help fine-tune the mitochondria (the powerhouse) of the cell, guiding them back into optimal performance. It assists the cell in removing toxins, lowering cellular stress caused by free radicals, and increasing the production of ATP, the molecule that stores and transports energy within the cell. The healthier, more energetic cells also produce other healthy cells when they replicate.
We use PEMF therapy because it can alleviate pain and inflammation, improve circulation, energy levels, and sleep quality, and promote cellular detoxification and regeneration. In addition to all these benefits, it decreases the recovery time needed for each of the other regenerative therapies while increasing their healing effects and providing the most healing support possible to the cells being targeted. In fact, it is so beneficial that PEMF is included as part of your treatment anytime you receive Ozone, OCM or Stem Cell injections at Temecula Center for Integrative Medicine.
Living with chronic pain is exhausting, and it is discouraging to believe that you face a future of merely learning to manage your pain. It is clear that chronic opioid use is not a good answer to help treat chronic pain. Regenerative Medicine and Functional Medicine provide treatment options that deal with the source of your problem and restore your body to health, rather than masking the pain with harmful, addictive medication or resorting to surgery which requires a long, painful recovery. Our treatments work with your body’s natural healing mechanisms to fix the root of your pain and discomfort. We specialize in treating complicated health issues and it is our mission to provide our patients with a deep healing experience so you can enjoy a healthy life, free from chronic pain.
Dr. Lundquist is Board Certified in Family Medicine with ABFM and he is sub-specialized with the American Board of Integrative Medicine (ABoIM). He has also has received a certification from the American Board of Integrative and Holistic Medicine (ABIHM).
Dr. Lundquist has a special interest in Integrative and Holistic medicine. He is currently the founder and medical director for the Temecula Center for Integrative Medicine specializing in all aspects of Functional Medicine. He is a member of the American Holistic Medical Association as well as the Institute of Functional Medicine. He specializes in endocrine disorders, especially thyroid and adrenal dysfunction, chronic fatigue, migraine headaches, cardio metabolic disorders, and chronic pain.
info@tcimedicine.com
951-383-4333
1. Baldini, A., Von Korff, M., & Lin, E. H. (2012). A Review of Potential Adverse Effects of Long-Term Opioid Therapy: A Practitioner's Guide. The primary care companion for CNS disorders, 14(3), PCC.11m01326. doi:10.4088/PCC.11m01326.
2. Krebs, E. E., Gravely, A., Nugent, S., Jensen, A. C., DeRonne, B., Goldsmith, E. S., … Noorbaloochi, S. (2018). Effect of Opioid vs Nonopioid Medications on Pain-Related Function in Patients With Chronic Back Pain or Hip or Knee Osteoarthritis Pain: The SPACE Randomized Clinical Trial. JAMA, 319(9), 872–882. doi:10.1001/jama.2018.0899.
3. Dublin, S., Walker, R. L., Jackson, M. L., Nelson, J. C., Weiss, N. S., Von Korff, M., & Jackson, L. A. (2011). Use of opioids or benzodiazepines and risk of pneumonia in older adults: a population-based case-control study. Journal of the American Geriatrics Society, 59(10), 1899–1907. doi:10.1111/j.1532-5415.2011.03586.x.
#drugs #functionalmedicine #regenerativemedicine #TCIM #chronicillness #stemcell #opioidcrisis #health #addiction #treatment #opioidaddiction #treatment